Study Notes

Overview
The study of stress is a cornerstone of health psychology and a significant component of the WJEC A-Level specification. It explores the body's intricate physiological response to perceived threats and the long-term consequences for our physical and mental health. For candidates, success in this topic hinges on a dual mastery: first, a precise understanding of the biological pathways, including the Sympathomedullary (SAM) system and the Hypothalamic-Pituitary-Adrenal (HPA) axis; and second, a robust ability to evaluate the research evidence linking stress to illness and the effectiveness of various management techniques. Examiners expect candidates to move beyond simple descriptions, applying theories to novel scenarios (AO2) and critically assessing the methodologies and conclusions of key studies (AO3). This guide will equip you with the detailed knowledge and analytical skills required to excel.
Key Concepts & Physiological Pathways
The Acute Stress Response: The SAM System
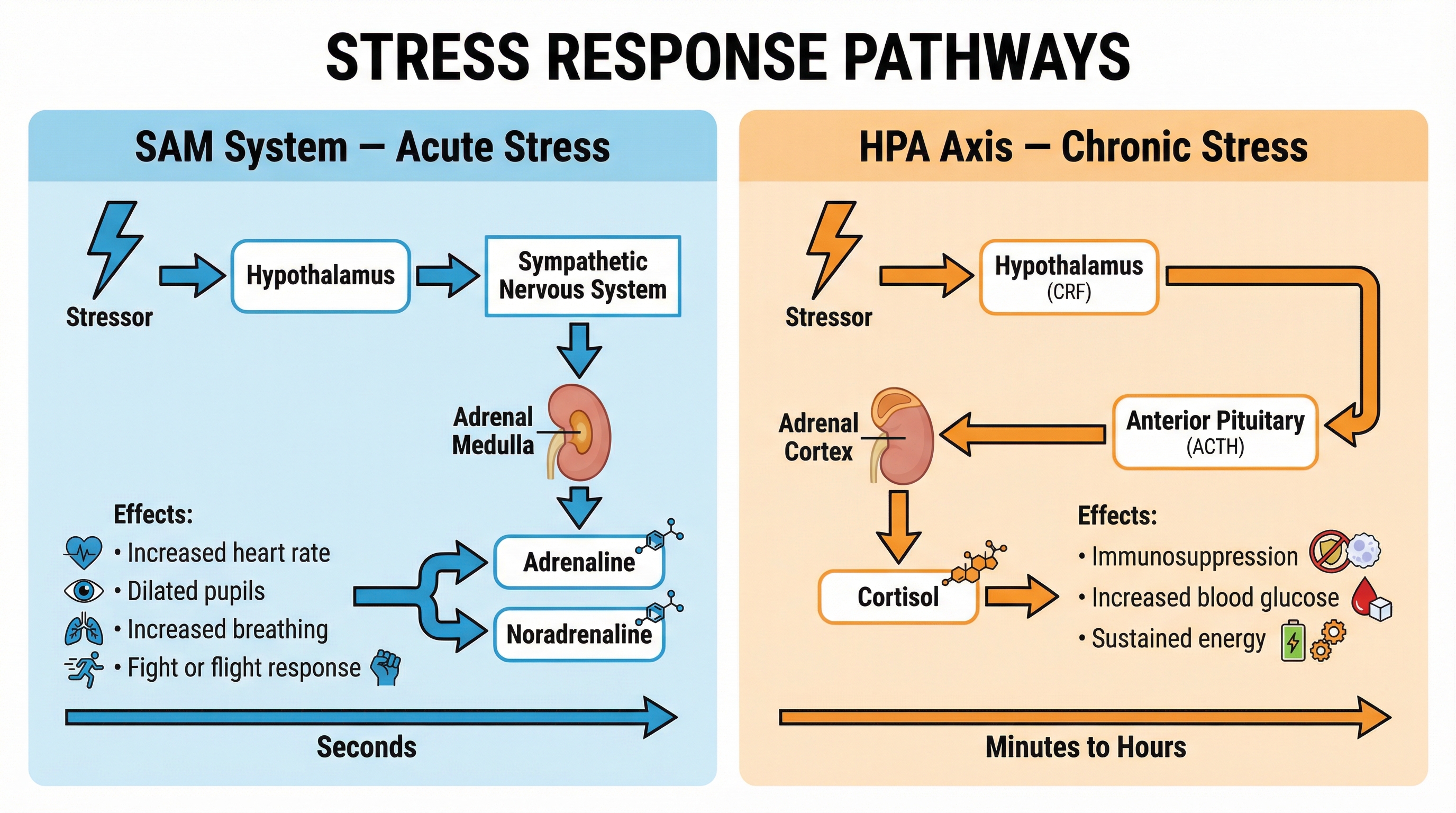
What happens: When an individual perceives a stressor as acute and immediate (e.g., a near-miss car accident), the hypothalamus activates the Sympathetic branch of the Autonomic Nervous System (ANS). This sends a neural signal to the Adrenal Medulla, which responds by releasing the catecholamines adrenaline and noradrenaline into the bloodstream. This is an incredibly fast process, preparing the body for immediate action.
Why it matters: This is the classic 'fight or flight' response. The surge of adrenaline and noradrenaline leads to increased heart rate, faster breathing, pupil dilation, and the diversion of blood to the muscles and away from non-essential functions like digestion. It provides a burst of energy and heightened alertness essential for survival. For the exam, candidates must be able to distinguish this pathway clearly from the HPA axis.
Specific Knowledge: Pathway: Hypothalamus → Sympathetic Nervous System → Adrenal Medulla → Adrenaline/Noradrenaline. Hormones: Adrenaline, Noradrenaline. Timescale: Seconds.
The Chronic Stress Response: The HPA Axis
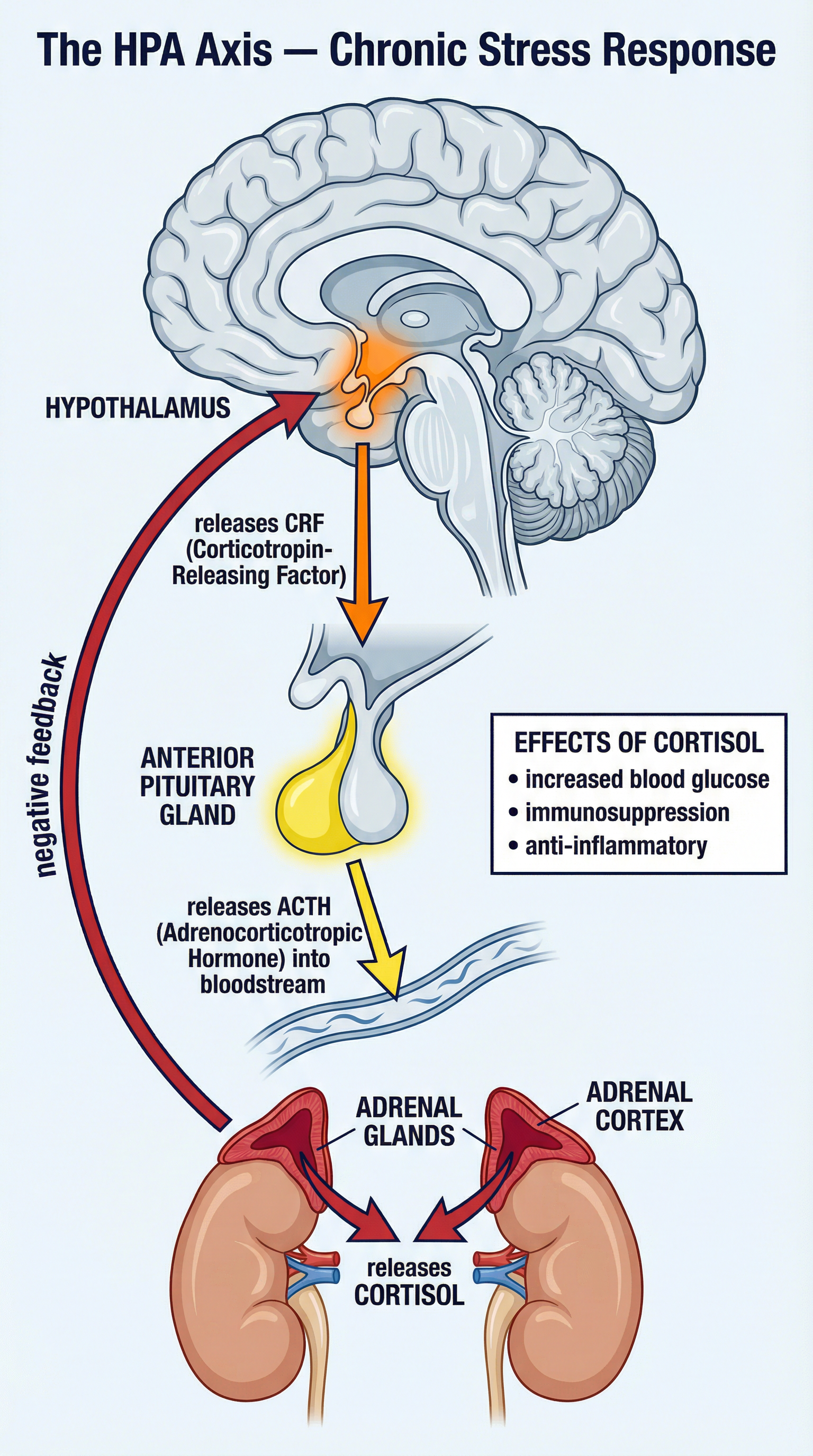
What happens: When a stressor is persistent or ongoing (e.g., long-term work pressure, exams), the body initiates a slower, longer-lasting response via the HPA axis. The hypothalamus releases Corticotropin-Releasing Factor (CRF). This is detected by the Anterior Pituitary gland, which in turn releases Adrenocorticotropic Hormone (ACTH). ACTH travels through the bloodstream to the Adrenal Cortex, stimulating it to release cortisol, a glucocorticoid hormone.
Why it matters: Cortisol plays a key role in managing chronic stress by maintaining a steady supply of blood sugar to provide energy over a sustained period. However, a major side effect of prolonged cortisol elevation is immunosuppression—the suppression of the immune system. This is the critical link between chronic stress and increased vulnerability to illness, a concept frequently tested in exams.
Specific Knowledge: Pathway: Hypothalamus (CRF) → Pituitary Gland (ACTH) → Adrenal Cortex → Cortisol. Hormone: Cortisol. Key Effect: Immunosuppression. Timescale: Minutes to hours.
Key Research Study
Kiecolt-Glaser et al. (1984) - Stress and Immunosuppression
Role: Provided the first direct evidence of stress-related immunosuppression in humans.
Key Actions: The researchers took blood samples from 75 first-year medical students (a naturally stressed group) one month before their final exams (low stress) and again during the exam period (high stress). They measured the activity of Natural Killer (NK) cells, a type of white blood cell crucial for fighting viruses and early cancers.
Impact: They found that NK cell activity was significantly lower during the high-stress period compared to the low-stress baseline. This demonstrated a measurable, negative impact of a common life stressor (academic exams) on immune function. This study is a cornerstone of psychoneuroimmunology and essential evidence for AO1 (description) and AO3 (evaluation) marks.
Individual Differences in Stress
Type A, B, and C Personalities
Concept: Friedman & Rosenman (1976) proposed that certain personality traits could predispose individuals to stress-related illness. Type A individuals are characterised by competitiveness, time urgency, and hostility. Type B individuals are more relaxed and patient. Later research identified Type C, characterised by bottling up emotions, particularly anger.
Impact: The Western Collaborative Group Study followed over 3000 men for 8.5 years and found that Type A men were twice as likely to develop coronary heart disease (CHD). However, later analysis suggests that the 'hostility' component is the most toxic element of the Type A personality, as it leads to a chronically over-active SAM response, increasing blood pressure and causing wear and tear on the cardiovascular system.
Hardiness
Concept: Kobasa (1979) identified a personality type that seems to be protective against the negative effects of stress. This 'hardy' personality consists of three elements, the 'Three Cs':
- Control: Hardy individuals have a strong sense of personal control over their lives (internal locus of control).
- Commitment: They are deeply involved in their work, relationships, and daily activities.
- Challenge: They view change and potential stressors as challenges to be overcome and opportunities for growth, rather than as threats.
Impact: Kobasa's research on business executives found that those who scored high on hardiness remained healthier despite experiencing high levels of stress. This concept is crucial for evaluation as it demonstrates that cognitive appraisal (how we interpret a stressor) is a critical mediator in the stress-illness relationship.
Stress Management Techniques
Biological Approaches (Drug Therapy)
- Benzodiazepines (BZs): Anti-anxiety drugs like Valium and Librium. They work by enhancing the action of the neurotransmitter GABA, which has a general quieting effect on many neurons in the brain, reducing anxiety. They are fast-acting but carry a high risk of tolerance and dependence.
- Beta-Blockers (BBs): Drugs like propranolol. They work by blocking the receptor sites for adrenaline and noradrenaline on the heart and other organs. This reduces the physiological arousal associated with the SAM response (e.g., lowered heart rate, reduced blood pressure). They are effective for performance anxiety but do not treat the underlying psychological cause of the stress.
Psychological Approaches (Cognitive Behavioural Therapy)
- Stress Inoculation Therapy (SIT): Developed by Meichenbaum (1985), this is a form of CBT that aims to give individuals the tools to 'inoculate' themselves against future stressors. It has three phases:
- Conceptualisation: The client and therapist identify the sources of stress and the client's current (often maladaptive) coping strategies.
- Skills Acquisition & Rehearsal: The client is taught a range of skills, such as relaxation, cognitive restructuring (challenging negative thoughts), and problem-solving. These are practised in the therapy session.
- Application & Follow-through: The client applies these newly learned skills in progressively more stressful real-world situations, often using imagery and role-playing first.
"